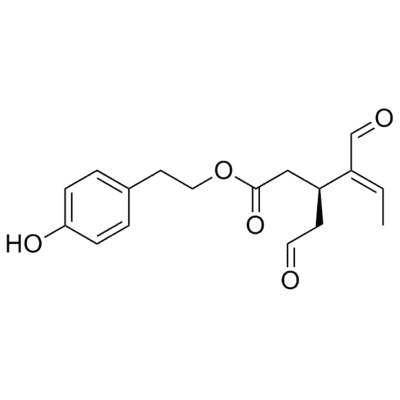
Oleocanthal is a type of natural phenolic compound found in extra-virgin olive oil.[1]
Healing Properties
Antiinflammatory
The anti-inflammatory activity of oleocanthal was initially investigated in relation to ibuprofen because these two compounds share similar chemical structure and cause a similar irritation in the oropharyngeal region. Interestingly, oleocanthal was found to be more potent than ibuprofen at inhibiting inflammatory enzymes.[2]
Anticancer
Brain Health (Neuroprotective)
Disease / Symptom Treatment
Alzheimer’s
Oleocanthal has been effective in counteracting two distinctive hallmarks of Alzheimer’s disease: neurofibrillary tangle and amyloid β deposition.[2:1]
- Oleocanthal inhibits the formation of hyperphosphorylated tau aggregates by interfering with the aggregation sites on tau protein.[2:2]
- Oleocanthal induces amyloid β efflux nd clearance by increasing P-glycoprotein ex-pression and activity and up-regulating low-density lipoprotein receptor-related protein.[2:3]
- Oleocanthal also stimulates amyloid β degradation inducing monomer degradation via up-regulation of the amyloid β degradation enzyme, adenosine triphosphate-binding cassette transporter-A1.[2:4]
- Oleocanthal also has the ability to modify the structure of amyloid β increasing its immunoreactivity.[2:5]
- Oleocanthal acts as an antioxidant agent.[2:6]
Breast Cancer
(−)‑oleocanthal (OLCT), a phenolic compound isolated from olive oil, impairs the ability of breast cancer cells to proliferate and migrate via downregulation of TRPC6 channel expression while having no effect on the biology of non-tumoral breast cells.[1:1]
Triple negative breast cancer
Triple negative breast cancer is an aggressive type of cancer that does not respond to hormonal therapy and current therapeutic strategies are accompanied by side effects due to cytotoxic actions on normal tissues.
Oleocanthal is an anti-cancer compound which can be used with negligible effects on non-tumoral cells.[1:2]
Title: (−)‑Oleocanthal inhibits proliferation and migration by modulating Ca2+ entry through TRPC6 in breast cancer cells
Author(s): R. Diez-Bello, I. Jardin, J.J. Lopez, M.El Haouari, J. Ortega-Vidal, J. Altarejos, G.M. Salidoa, S. Salido, J.A. Rosado
Institution(s): Department of Physiology (Cellular Physiology Research Group), Institute of Molecular Pathology Biomarkers, University of Extremadura, 10003 Caceres, Spain; Centre Régional des Métiers de l’Education et de la Formation de Taza, 35000 Taza, Morocco; Laboratoire Matériaux, Substances Naturelles, Environnement & Modélisation (LMSNEM), Faculté Polydisciplinaire de Taza, Université Sidi Mohamed Ben Abdellah, Fès, Morocco; Department of Inorganic and Organic Chemistry, University of Jaen, Campus de Excelencia Internacional Agroalimentario (ceiA3), 23071 Jaen, Spain
Publication: Biochimica et Biophysica Acta (BBA) - Molecular Cell Research
Date: October 2018
Abstract: Triple negative breast cancer is an aggressive type of cancer that does not respond to hormonal therapy and current therapeutic strategies are accompanied by side effects due to cytotoxic actions on normal tissues. Therefore, there is a need for the identification of anti-cancer compounds with negligible effects on non-tumoral cells. Here we show that (−)‑oleocanthal (OLCT), a phenolic compound isolated from olive oil, selectively impairs MDA-MB-231 cell proliferation and viability without affecting the ability of non-tumoral MCF10A cells to proliferate or their viability. Similarly, OLCT selectively impairs the ability of MDA-MB-231 cells to migrate while the ability of MCF10A to migrate was unaffected. The effect of OLCT was not exclusive for triple negative breast cancer cells as we found that OLCT also attenuate cell viability and proliferation of MCF7 cells. Our results indicate that OLCT is unable to induce Ca2+ mobilization in non-tumoral cells. By contrast, OLCT induces Ca2+ entry in MCF7 and MDA-MB-231 cells, which is impaired by TRPC6 expression silencing. We have found that MDA-MB-231 and MCF7 cells overexpress the channel TRPC6 as compared to non-tumoral MCF10A and treatment with OLCT for 24–72 h downregulates TRPC6 expression in MDA-MB-231 cells. These findings indicate that OLCT impairs the ability of breast cancer cells to proliferate and migrate via downregulation of TRPC6 channel expression while having no effect on the biology of non-tumoral breast cells.
Link: Source
Citations:
Title: New neuroprotective perspectives in fighting oxidative stress and improving cellular energy metabolism by oleocanthal
Author(s): Cristina Angeloni, Laura Giusti, Silvana Hrelia PhD
Institution(s): School of Pharmacy, University of Camerino, Camerino, Italy; Department of Clinical and Experimental Medicine, University of Pisa, Pisa, Italy; Department for Life Quality Studies, Alma Mater Studiorum - University of Bologna, Rimini, Italy
Publication: Neural Regeneration Research
Date: October 2018
Abstract: Neurodegenerative diseases are a heterogeneous group of disorders characterized by a progressive dysfunction and death of neural cells which lead to compromised motor or cognitive function. Morphologically, the loss of neuron is associated with both gliosis and, frequently, with abnormal accumulation of extracellular and intracellular filamentous deposit in specific cell types. With a rapidly increasing aging population, these diseases are becoming a primary health problem (Albers and Beal, 2000). Neurodegenerative diseases have been considered to be interplay of a number of factors, however mounting evidence suggests that a rise in oxidative stress may play a critical role in the pathogenesis of many of these disorders like Alzheimer’s disease, Parkinson’s disease, amyotrophic lateral sclerosis, and Huntington’s disease (Li et al., 2013). It has been observed that the abnormal protein aggregation that characterizes many neurodegenerative diseases can in turn activate inflammation in the brain, which triggers a strong release of reactive oxygen species and reactive nitrogen species, subsequent oxidative and nitrosative stress and, eventually, cell death. It has been observed that the principal mode of neuronal cell death in neurodegenerative diseases is via apoptosis (Liu et al., 2017)
Link: Source
Citations: